Living Pain-Free: Your Essential Guide to Chronic Low Back Pain
Up to 84% of adults will experience low back pain at some point in their lives. However, for many, this isn’t just a temporary inconvenience – chronic low back pain can become a debilitating condition that significantly impacts daily activities and quality of life.
In fact, approximately 23% of adults worldwide suffer from chronic lower back pain, making it one of the most common musculoskeletal complaints we see at IROSM. This condition represents 30% of sick leaves lasting longer than 6 months and has become the leading cause of work exclusion before age 45. Furthermore, the economic burden is substantial, with annual costs estimated between $12.2 and $90.6 billion.
Whether you’re dealing with persistent lower back pain symptoms or seeking effective lower back pain relief, understanding the underlying causes and treatment options is essential. As an interventional pain specialist, Dr. Michael Erdman recognizes that most patients with chronic low back pain will not benefit from surgery. Instead, the goals of treatment often shift from initially seeking a cure to improving pain and function over time.
In this comprehensive guide, we’ll explore what causes lower back pain, how it’s diagnosed, and the most effective treatments for chronic back pain – from non-pharmacologic approaches to medication and interventional options. Our goal is to help you understand your condition and find a path toward living pain-free.
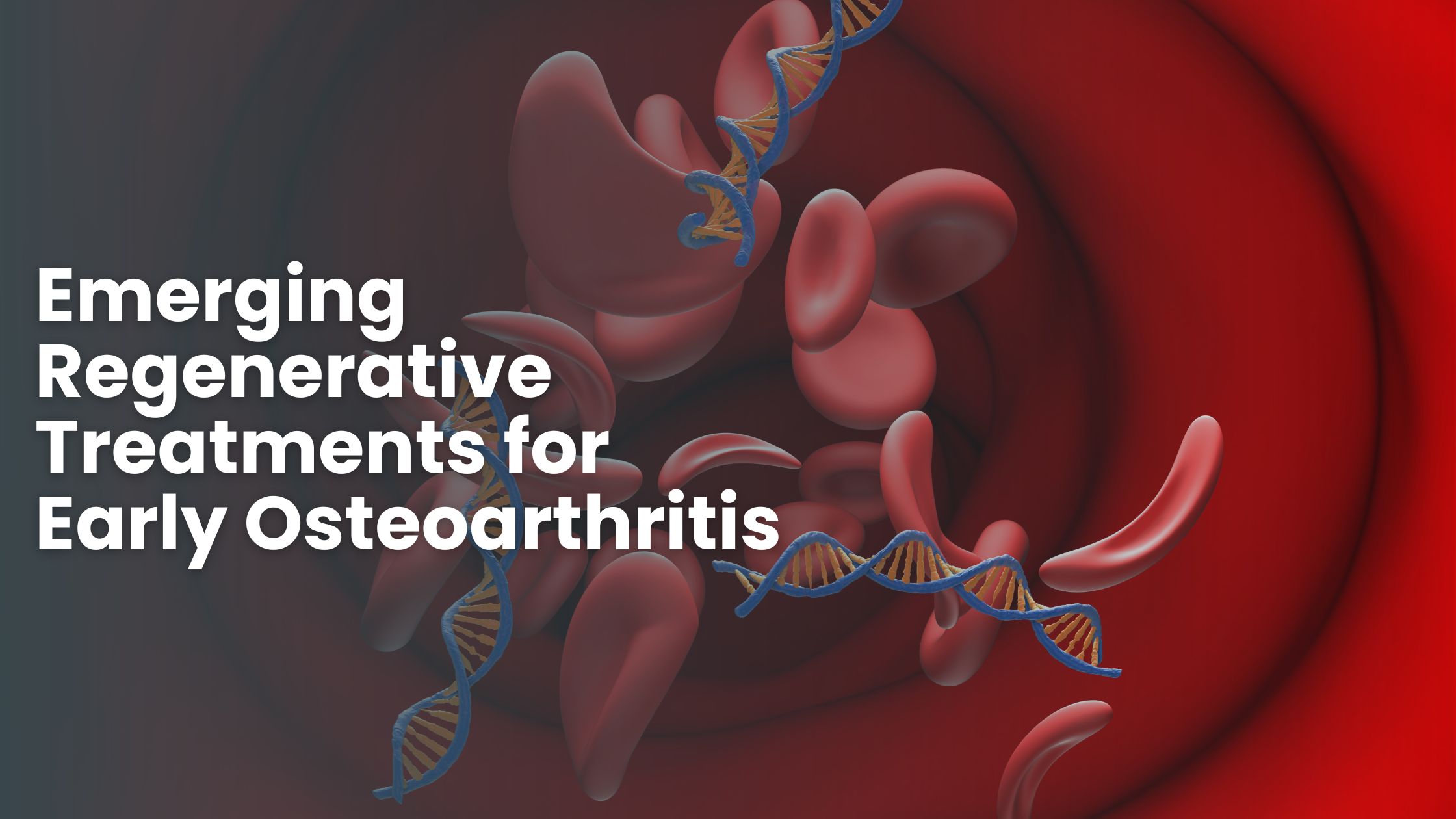
Understanding Chronic Low Back Pain
Image Source: WebMD
“Pain is a construct of the brain – 100% of the time.” — Dr Lorimer Moseley, Clinical scientist investigating pain in humans, co-author of ‘Explain Pain’
Chronic low back pain isn’t just a persistent ache—it’s a complex condition that affects millions of people worldwide. Although most back pain resolves quickly, understanding why some cases become chronic is essential for finding effective solutions.What makes pain ‘chronic’?
Pain officially becomes “chronic” when it persists for more than 12 weeks (3 months) [1][2]. Unlike acute pain that serves as a warning signal, chronic pain continues long after the initial injury has healed. Approximately 5-10% of low back pain cases develop into chronic conditions [2].
Some experts describe chronic back pain as occurring on less than half the days in a 12-month period, appearing in multiple episodes throughout the year [3]. Additionally, others define it as pain that comes and goes—flaring up periodically but generally worsening over time [4].
Common lower back pain symptoms
Low back pain can manifest in various ways, ranging from mild, dull discomfort to severe, disabling pain [5]. You might experience:
- Pain characteristics: Sharp or dull aching, burning, stabbing, or throbbing sensations [1]
- Radiation: Pain that spreads to your buttocks, hips, or travels down one or both legs [6][7]
- Movement limitations: Stiffness, decreased range of motion, or difficulty standing straight [4]
- Muscle issues: Sudden spasms or contractions that can be extremely painful [4]
Many people notice their symptoms worsen with specific activities like sitting, standing, bending, or lifting [6]. Morning stiffness is also common, with pain sometimes improving with gentle movement [7].
Why does my lower back hurt?
Interestingly, chronic lower back pain often develops without a clear cause that shows up on imaging tests [6]. While acute pain typically stems from muscle or ligament injuries, chronic pain usually involves issues with the spine’s discs, nerves, joints, or vertebrae [4].
Common underlying causes include:
- Osteoarthritis and degenerative disc disease [4]
- Bulging or ruptured discs pressing on nerves [6]
- Spinal stenosis (narrowing of spaces within your spine) [2][6]
- Structural problems like scoliosis [8]
Several factors can increase your risk, such as being over 30, carrying excess weight, experiencing high stress levels, or working in occupations that require heavy lifting [8].
Understanding the complexity of chronic low back pain is the first step toward effective management and finding appropriate treatment options.
How Chronic Low Back Pain is Diagnosed
Diagnosing chronic low back pain requires a comprehensive approach that goes beyond simply identifying pain. Healthcare providers utilize specific assessment methods to determine appropriate treatment paths.
Red flags: when to worry
Certain symptoms warrant immediate medical attention as they may indicate serious underlying conditions. These “red flags” include:
- Severe or progressive neurological deficits (including bladder/bowel dysfunction)
- Fever or recent infection
- Unexplained weight loss
- History of cancer or strong suspicion for current cancer
- Significant trauma or osteoporosis with minor fall
- Age over 50 with new-onset pain [9][10]
Specifically, cauda equina syndrome—characterized by saddle anesthesia, loss of bowel/bladder control, or progressive leg weakness—requires emergency evaluation [11].
Yellow, blue, and black flags explained
Beyond physical causes, psychosocial factors often predict chronicity. “Yellow flags” refer to psychological risk factors like fear-avoidance beliefs, catastrophizing, and anxiety [2]. Meanwhile, “blue flags” relate to workplace perceptions—job satisfaction, stress levels, and support at work [12]. “Black flags” encompass system obstacles outside a patient’s control: insurance issues, company policies, or societal factors [8].
The role of imaging and physical exams
Physical examination typically includes assessment of posture, range of motion, neurological function, and specific tests like the straight leg raise [13]. Despite technological advances, imaging is not recommended for most patients within the first 6 weeks unless red flags are present [14]. Unnecessary imaging can lead to poorer outcomes and increased surgeries—one study found patients receiving early MRIs were eight times more likely to undergo surgery without improved recovery [15].
Screening tools: STarT Back and Örebro
Two validated tools help identify patients at risk for persistent problems. The STarT Back Screening Tool categorizes patients into three risk groups (low, medium, high), guiding treatment decisions [16]. This approach has been shown to decrease disability and reduce healthcare costs [17]. Similarly, the Örebro Musculoskeletal Pain Screening Questionnaire predicts future work disability—patients in the high-risk group demonstrated 7.5 times more sick leave days and 16-fold higher odds of disability pension during follow-up [18].
Non-Pharmacologic Treatments That Work
“I don’t believe in pain management anymore, I believe in trying to cure persistent pain.” — Dr. Howard Schubiner, Physician, pain specialist, author
Non-pharmacologic approaches form the cornerstone of effective chronic low back pain management. Research consistently shows these treatments can provide substantial relief without the risks associated with medications or surgery.Exercise therapy and physical activity
Exercise remains the foundation of chronic back pain treatment and is recommended as first-line care by clinical practice guidelines [5]. Various exercise types benefit patients with chronic low back pain, including:
- Core strengthening and stabilization exercises
- Aerobic activities (walking, swimming, cycling)
- Flexibility and stretching routines
- Mind-body practices (yoga, tai chi, Pilates)
No single exercise regimen proves superior to others [5]. Therefore, clinicians should consider individual preferences, needs, and capabilities when prescribing an exercise program [1]. Regular physical activity not only reduces pain intensity but essentially improves functional status, enhances sleep quality, and diminishes fear-avoidance beliefs [19].
Physiotherapy and manual therapy
Manual therapy involves hands-on techniques aimed at relaxing tense muscles and mobilizing restricted joints [20]. Common approaches include spinal manipulation, soft tissue mobilization, and massage. These techniques primarily work by decreasing back pain through improved joint mobility and reduced muscle tension [20].
Studies show massage therapy can provide long-lasting benefits, with improvements observed even at one-year follow-up [21]. Moreover, combining manual therapy with targeted exercises often yields better outcomes than either approach alone [22].
Cognitive behavioral therapy (CBT)
CBT addresses the psychological aspects of chronic pain through a structured approach that typically involves six phases: assessment, reconceptualization, skills acquisition, skills consolidation, generalization, and follow-up [23]. This therapy helps patients replace maladaptive coping strategies with more effective ones [23].
Research demonstrates CBT’s effectiveness in improving pain control, reducing disability, and enhancing overall function [24]. Consequently, CBT remains valuable for addressing pain-related anxiety, catastrophizing thoughts, and sleep disturbances [7].
Patient education and self-management
Education about chronic low back pain serves as critical first-line care [25]. Even brief educational interventions (as short as five minutes) can benefit patients for up to 12 months [25]. Effective education helps patients understand their condition, reduces unnecessary healthcare use, and empowers them to manage symptoms independently [25].
Self-management support should focus on building problem-solving skills and improving self-efficacy rather than emphasizing pain and impairment [26]. This approach encourages patients to take an active role in their recovery process.
Multidisciplinary rehabilitation programs
For complex cases, multidisciplinary biopsychosocial rehabilitation combines physical, psychological, and social/work-targeted components [27]. These programs typically involve healthcare providers from different specialties working together toward comprehensive pain management [27].
Research indicates multidisciplinary approaches yield superior results compared to usual care, with moderate-quality evidence showing improvements in pain, disability, and return-to-work outcomes [27]. Their effectiveness stems from addressing the biological, psychological, and social factors that contribute to chronic pain.
Pharmacologic and Interventional Options
Medication and interventional procedures often play important roles in managing chronic low back pain, particularly when non-pharmacologic approaches provide insufficient relief. Understanding the evidence behind these options helps in making informed treatment decisions.
First-line medications: NSAIDs and acetaminophen
NSAIDs remain among the most frequently prescribed medications for mechanical low back pain worldwide [28]. They provide modest benefits through their anti-inflammatory effects, with studies showing NSAIDs are more effective than placebo for chronic low back pain, though the difference is small—only about 7 points on a 100-point pain scale [28]. Notably, different types of NSAIDs appear equally effective [6].
Acetaminophen (Tylenol) works differently, primarily affecting the central nervous system rather than reducing inflammation [4]. Contrary to common belief, recent evidence suggests acetaminophen may not be better than placebo for acute low back pain [29]. Yet, it remains valuable for patients unable to tolerate NSAIDs due to its favorable safety profile [30].
When to consider opioids or antidepressants
Opioids should typically be considered a last resort for chronic low back pain [4]. Research indicates they may not be superior to non-opioid medications—one study found opioid therapy wasn’t better than non-opioid medication for improving pain-related function over 12 months [31]. Furthermore, the risks of addiction, tolerance, and side effects often outweigh potential benefits [4].
Antidepressants, particularly duloxetine (Cymbalta), have shown promise in managing chronic low back pain even without depression [32]. A recent analysis found duloxetine 60mg significantly reduced pain compared to placebo [32]. Tricyclic antidepressants like amitriptyline are commonly prescribed (48.4% of all amitriptyline prescriptions are for pain) [3], yet evidence supporting their effectiveness remains limited [33].
Topical treatments: what helps and what doesn’t
Topical analgesics offer localized relief with fewer systemic side effects. Diclofenac gel demonstrates good evidence of effectiveness for musculoskeletal pain [34]. Likewise, topical lidocaine and capsaicin may benefit some patients—a study found over-the-counter 3.6% lidocaine combined with menthol was as effective as prescription 5% lidocaine patches [29].
Spinal injections: when are they appropriate?
Epidural steroid injections target inflammation around spinal nerves [35]. They’re most appropriate for radicular pain (sciatica) caused by conditions like herniated disks or spinal stenosis [35]. Nonetheless, evidence suggests these injections typically provide only temporary relief lasting about three months [35]. Indeed, a systematic review found epidural injections were only marginally more effective than placebo in reducing leg pain at short-term follow-up [36].
Apart from epidural injections, facet joint injections and sacroiliac joint injections may benefit selected patients whose pain originates from these specific structures [37].
Meet Dr. Michael Erdman
Interventional Pain Management Physician
Dr. Michael Erdman, a fellowship-trained interventional pain specialist, provides advanced, non-surgical treatments for acute and chronic pain in Fort Lauderdale, Miami, and surrounding areas.
Fluent in English and Spanish, Dr. Erdman offers personalized care for conditions like back and neck pain, sciatica, arthritis, and post-surgical discomfort. Treatments include image-guided injections, radiofrequency ablation, and regenerative therapies like PRP and stem cells performed in-office with precision and care.
Now accepting patients across Broward and Miami-Dade Counties.

Conclusion
Living with chronic low back pain presents significant challenges, yet effective management remains possible through a comprehensive approach. Throughout this guide, we’ve explored the complexity of this condition that affects nearly a quarter of adults worldwide. Certainly, most cases won’t require surgery, shifting our focus toward improving function and quality of life rather than seeking an absolute cure.
Understanding the transition from acute to chronic pain helps patients recognize why their symptoms persist beyond the typical healing period. Pain characteristics vary widely, from dull aches to sharp, radiating sensations that significantly impact daily activities. Additionally, proper diagnosis proves crucial, with healthcare providers carefully assessing red flags that might indicate serious underlying conditions while considering psychological and social factors that influence recovery.
Non-pharmacologic treatments undoubtedly form the cornerstone of effective management. Exercise therapy stands out as particularly beneficial, regardless of the specific type chosen. Similarly, physiotherapy, cognitive behavioral therapy, and patient education empower individuals to take control of their condition. For complex cases, multidisciplinary rehabilitation programs address the biological, psychological, and social aspects simultaneously.
Medication and interventional approaches serve as adjunctive options when other treatments provide insufficient relief. NSAIDs offer modest benefits, while opioids should generally remain a last resort due to their limited long-term effectiveness and potential risks. Spinal injections might provide temporary relief for specific conditions but rarely offer permanent solutions.
Above all, we believe successful management of chronic low back pain requires active participation. Rather than passively receiving treatments, patients who engage in self-management strategies and work collaboratively with healthcare providers typically experience better outcomes. The journey toward living pain-free may not always follow a straight path, but with appropriate care and persistence, significant improvements remain achievable for most people suffering from this common condition.
Key Takeaways
Chronic low back pain affects 23% of adults worldwide and becomes a complex condition requiring comprehensive management rather than seeking a simple cure.
• Exercise is your best medicine: Any type of regular physical activity—from walking to yoga—provides the strongest evidence for reducing chronic back pain and improving function.
• Most imaging is unnecessary: MRIs and X-rays within the first 6 weeks often lead to worse outcomes and unnecessary surgeries without improving recovery.
• Psychology matters as much as anatomy: Fear-avoidance beliefs, catastrophizing, and workplace stress often predict who develops chronic pain more than physical findings.
• Medications have limited long-term benefits: NSAIDs provide only modest relief (7 points on 100-point scale), while opioids show no superiority over non-opioid treatments.
• Red flags require immediate attention: Bladder/bowel dysfunction, progressive weakness, fever, or unexplained weight loss warrant emergency medical evaluation.
• Multidisciplinary care works best: Combining physical therapy, education, psychological support, and self-management strategies yields superior results to single treatments alone.
The path to living pain-free requires active participation in your care, focusing on function improvement over complete pain elimination, and working collaboratively with healthcare providers who understand the biopsychosocial nature of chronic pain.
FAQs
Q1. How long does back pain need to last to be considered chronic? Back pain is typically considered chronic when it persists for more than 12 weeks or 3 months. Some experts also describe it as pain that occurs on less than half the days in a 12-month period, appearing in multiple episodes throughout the year.
Q2. What are the most effective non-pharmacological treatments for chronic low back pain? The most effective non-pharmacological treatments include regular exercise (such as core strengthening, aerobic activities, and flexibility routines), physiotherapy, cognitive behavioral therapy, and patient education. Multidisciplinary rehabilitation programs that address physical, psychological, and social factors have also shown superior results.
Q3. When should I be concerned about my lower back pain? You should seek immediate medical attention if you experience “red flag” symptoms such as severe or progressive neurological deficits, fever, unexplained weight loss, history of cancer, or loss of bowel/bladder control. These could indicate serious underlying conditions requiring urgent evaluation.
Q4. Are pain medications the best solution for chronic low back pain? While medications like NSAIDs can provide modest relief, they are not considered the best long-term solution for chronic low back pain. Non-pharmacologic approaches, particularly exercise and physical activity, are recommended as first-line treatments. Opioids should typically be considered a last resort due to their limited long-term effectiveness and potential risks.
Q5. How important is self-management in dealing with chronic low back pain? Self-management is crucial in effectively dealing with chronic low back pain. Patient education and developing problem-solving skills are essential components of treatment. Individuals who actively participate in their care and engage in self-management strategies typically experience better outcomes than those who rely solely on passive treatments.
References
[1] – https://www.iasp-pain.org/resources/fact-sheets/exercise-and-chronic-low-back-pain/
[2] – https://academic.oup.com/ptj/article/91/5/737/2735759
[3] – https://www.bmj.com/content/372/bmj.m4825
[5] – https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD009790.pub2/full
[6] – https://www.cochrane.org/evidence/CD000396_non-steroidal-anti-inflammatory-drugs-low-back-pain
[7] – https://pmc.ncbi.nlm.nih.gov/articles/PMC4671906/
[8] – https://pmc.ncbi.nlm.nih.gov/articles/PMC5741323/
[9] – https://pmc.ncbi.nlm.nih.gov/articles/PMC7529135/
[10] – https://www.aafp.org/pubs/afp/issues/2018/1001/p421.html
[12] – https://www.physio-pedia.com/The_Flag_System
[13] – https://my.clevelandclinic.org/health/diseases/7936-lower-back-pain
[14] – https://pmc.ncbi.nlm.nih.gov/articles/PMC6118107/
[16] – https://www.physio-pedia.com/STarT_Back_Screening_Tool
[17] – https://startback.hfac.keele.ac.uk/
[18] – https://pmc.ncbi.nlm.nih.gov/articles/PMC10234666/
[19] – https://pmc.ncbi.nlm.nih.gov/articles/PMC6251828/
[20] – https://www.spine-health.com/treatment/physical-therapy/manual-physical-therapy-pain-relief
[21] – https://www.va.gov/WHOLEHEALTHLIBRARY/tools/non-drug-approaches-to-chronic-pain.asp
[22] – https://www.jospt.org/doi/10.2519/jospt.2021.0508
[23] – https://pmc.ncbi.nlm.nih.gov/articles/PMC3237294/
[24] – https://www.abct.org/fact-sheets/low-back-pain/
[25] – https://www.iasp-pain.org/resources/fact-sheets/back-pain-education/
[26] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8353288/
[27] – https://www.bmj.com/content/350/bmj.h444
[28] – https://pmc.ncbi.nlm.nih.gov/articles/PMC7104791/
[29] – https://pmc.ncbi.nlm.nih.gov/articles/PMC8119578/
[30] – https://www.spine-health.com/treatment/pain-medication/acetaminophen-back-pain
[31] – https://jamanetwork.com/journals/jama/fullarticle/2673971
[32] – https://pubmed.ncbi.nlm.nih.gov/39377458/
[34] – https://pmc.ncbi.nlm.nih.gov/articles/PMC6481750/
[35] – https://my.clevelandclinic.org/health/treatments/22091-lumbar-epidural-steroid-injection
[37] –https://orthoinfo.aaos.org/en/treatment/spinal-injections/